A Strange Case of Chest Pain and Hypotension
Mar 24, 2024The CASE
52 yo with chest pain and hypotension
It’s a busy afternoon in a rural emergency department and the ambulance bring in a 52 yo with central chest pain and a blood pressure of 70/45.
His past medical history is of an LAD blockage for which he has had a stent and then a redo of that stent.
He is complaining of pain that is central and pressing and 3/10, not sudden onset and no radiation. There is some change with inspiration, but minor. The pain started approximately 2 hours previously.
Medications included Aspirin, Clopidogrel and a Ca channel blocker that he had been taking since the stents. He had no allergies.
On Examination the patient looks well and is in no distress.
Vitals are HR 62bpm, BP 70/45, Sats 97% on room air. Blood Pressure and pulses were equal in both arms.
Heart sounds are dual and chest is clear and abdomen soft, with no pulsatile masses.
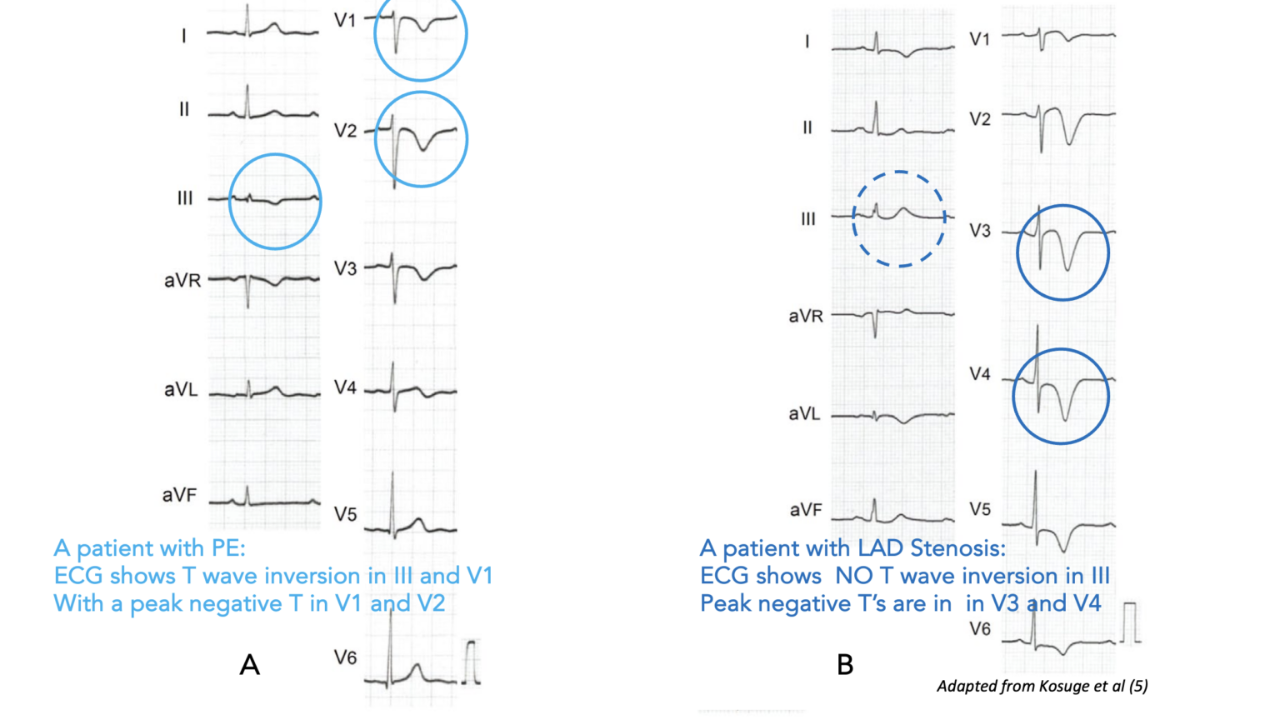
His initial ECG is shown below:

ECG summary and Diagnosis
In most cases we would describe this as an ischaemic ECG and would call it Wellen's Syndrome.
There are some important differences in Wellens.
Characteristics of Wellen’s Syndrome are:
- Recent chest pain history
- Cardiac Enzymes normal or minimally elevated
- Deep T waves or biphasic T wave in V2-V5 in pain free period
- No Q waves
- No Loss of R waves
- Minimal ST elevation
A quick search of the patient’s previous presentation demonstrated the same pattern on ECG.
How would you initially resuscitate this patient with low BP?
- IV Fluids? If so how much?
- Metaraminol?
- Adrenaline (epinephrine)?
- Noradrenaline (norepinephrine)?
Initial Resuscitation: What we did and why
Other investigations
The patient had a mobile chest xray which was normal. Lung fields were clear and mediastinum within normal limits.
By this time the high sensitivity troponin had returned and was normal.
A bedside cardiac echo was performed which did not show a pericardial effusion, nor was there right atrial dilatation, initially showing no evidence of cardiac tamponade and a lower risk of pulmonary embolism (definitive imaging was needed). This was a difficult study due to the patient’s body habits. The fact that there was no pericardial effusion, also contributed to our thinking that there may not be a proximal aortic dissection (further imaging was done) As the patient’s blood pressure stabilised with the noradrenaline infusion a CT was performed to look for a pulmonary embolism and any evidence of a dissection.
The Causes of Shock
The next thing we did was go over the causes of shock mnemonic.
SHOCKED
SEPSIS
The patient was obviously not in septic shock
HAEMORRHAGE/HYPOVOLAEMIA
There was no haemorrhage or hypovolaemia, however 1litre of crystalloid was given, which made no difference to the blood pressure, except transiently.
OBSTRUCTION
A bedside cardiac echo was performed originally gave us adequate information to say there was a lower risk of cardiac tamponade and a pulmonary embolism and to a lesser extent a dissection. As the patient’s blood pressure stabilised with the noradrenaline infusion a CT was performed to look for a pulmonary embolism and any evidence of a dissection. This was clear.
CARDIAC
A cardiac cause was our working diagnosis
ANAPHYLAKSIS
This was not a case of anaphylaxis
ENDOCRINE CAUSES
There was no history of endocrine disease and no abnormality of Na or K. It was assumed that there was no adrenal issue at this point, so no steroids were give. Perhaps a single dose should have been given.
DRUGS
The patient was asked about overdose but denied this.
What Happened Next?
The assumption was that the patient was having an ischaemic episode with a potential LAD stent blockage. His blood pressure was stabilised and he was transferred to a tertiary institution where the original two stents had been placed.
On arrival to the institution a coronary angiogram was performed, which showed patent stents and no other coronary lesions. It was assumed that the ECG changes were chronic.
The patient’s then progressively became more hypotensive and required an increasing noradrenaline dosage, almost to maximum. This progressively was weaned over the next 24 hours.
The patient then became significantly bradycardic and required pacing wires to be inserted. The pacing requirement also decreased within the next 24 hours.
Over the following 24 hours he developed significant cardiac failure and required intubation.
Scans again confirmed no Pulmonary embolism or dissection. Echo revealed some septal motion abnormalities.
On speaking to the doctor who had treated him on previous occasions, it was discovered that the patient had taken a previous overdose of beta blockers and had presented to an ED in a similar way, without admitting to taking the overdose.
The working diagnosis is Calcium Channel Overdose.
How do patients usually present with general Ca channel overdose?

Treatment
Decontamination: Activated Charcoal 50g if alert and:
- Standard Release
- < 2hours post ingestion
- Modified Release
- < 6hours of Amlodipine / Nifedipine / Felodipine / Lercanidipine / Nimodipine
- < 12 hours of Verapamil / Diltiazem
Bradycardia
- Atropine: 0.6mg (paeds 0.02mg/kg) IV x 3 doses q 5min
- Pacing
Hypotension
- Fluids: 10-20mL/kg crystalloid- beware as too much fluid can cause pulmonary oedema.
- Pressors: Noradrenaline as first line agent, unless bradycardia, then Adrenaline can be used. If using Noradrenaline and not effective can add Vasopressin
- Calcium: 30 mL Ca gluconate 10% (3 grams, 6.6 mmol) IV over 10 minutes x 3 in 60 minutes. Then Ca infusion to maintain ionized Ca2+ concentration 1.5 – 2.0 mmol/L
- High Dose Insulin Euglycaemic Therapy (Discuss with Toxicology)
- Actrapid 1u/kg IV then infusion +50 ml of 50% dext then infusion
- Sodium Bicarbonate: 1-2 mmol/kg 3-5 min to PH >7.3
- Methylene Blue / Lipid Emulsion in refractory shock (Discuss with Toxicology)
- ECMO if hypotension is refractory to all treatments
Join Our Free email updates
Get breaking news articles right in your inbox. Never miss a new article.
We hate SPAM. We will never sell your information, for any reason.